COBRA Continuation Coverage Election Form
Overview of this form
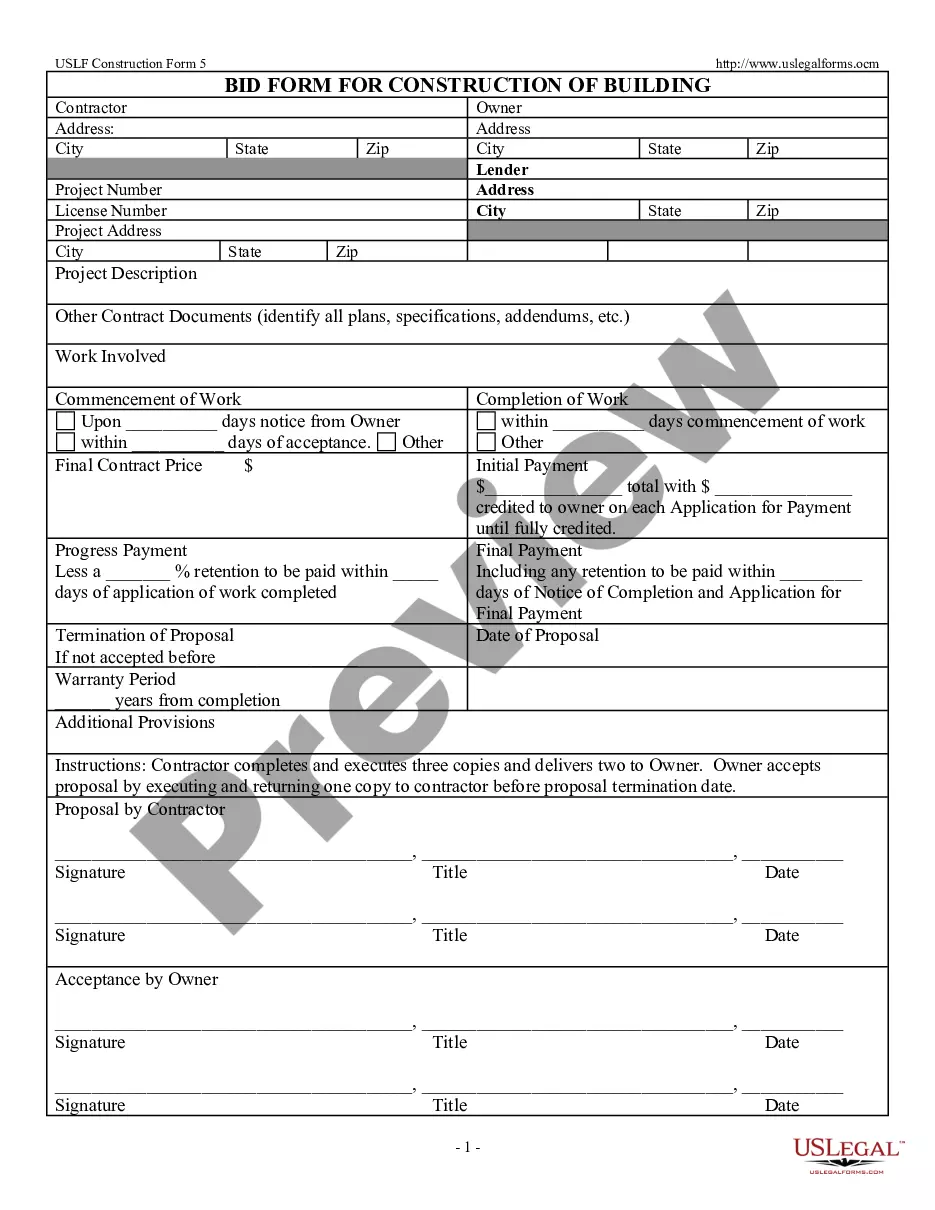
The COBRA Continuation Coverage Election Form is a legal document that allows individuals to elect to continue their health insurance coverage under the Consolidated Omnibus Budget Reconciliation Act (COBRA). This form is essential for those who have recently experienced a qualifying event that affects their health benefits. Unlike standard insurance application forms, this document specifically pertains to the continuation of healthcare coverage after losing group insurance due to job loss or other qualifying circumstances.
Form components explained
- Election deadline: Specifies the 60-day period for submitting the form after receiving the notice.
- Submission details: Provides the name and address where the form must be sent or instructions for submitting electronically.
- Coverage information: Identifies the specific health plan for which coverage is being elected.
- Election options: Allows the individual to choose which dependents will continue their coverage.
- Signature field: Requires the signature of the individual electing COBRA coverage.
Situations where this form applies
You should use the COBRA Continuation Coverage Election Form if you have lost your employer-sponsored health insurance due to qualifying events such as termination of employment, reduction in hours, or other events that result in loss of health benefits. Completing this form is necessary to ensure you can maintain your health coverage without interruption, particularly during challenging transitions.
Who should use this form
- Individuals who have recently been laid off or terminated from their job.
- Employees who have experienced a change in work hours that affects health benefits.
- Qualified dependents of the covered employee who wish to continue their coverage.
Completing this form step by step
- Fill out your personal information accurately, including your name, address, and contact information.
- Specify the health plan you are electing to continue coverage for, as indicated on the notice.
- List any dependents you wish to include in the coverage.
- Sign and date the form to confirm your election for COBRA continuation coverage.
- Submit the form via mail or any other specified means before the deadline provided in your notice.
Notarization guidance
Notarization is generally not required for this form. However, certain states or situations might demand it. You can complete notarization online through US Legal Forms, powered by Notarize, using a verified video call available anytime.
Get your form ready online
Our built-in tools help you complete, sign, share, and store your documents in one place.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.
Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.
Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.

Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.

Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Common mistakes
- Failing to submit the form by the deadline.
- Neglecting to sign the form, making it invalid.
- Not including all eligible dependents on the form.
- Submitting the form to an incorrect address or via the wrong method.
Benefits of completing this form online
- Convenience: Access and complete the form at your own pace from any location.
- Editability: Easily make changes if needed before finalizing your submission.
- Guidance: Receive supportive instructions to help you fill out the form correctly.
Summary of main points
- The COBRA form is crucial for maintaining health insurance coverage after employment changes.
- Timeliness is essential; submit your Election Form within 60 days of receiving your notice.
- Be thorough and accurate when filling out personal details and plan information.
Looking for another form?
Form popularity
FAQ
Notifying all eligible group health care participants of their COBRA rights. Providing timely notice of COBRA eligibility, enrollment forms, duration of coverage and terms of payment after a qualifying event has occurred.
Leave a company with 20 or more employees, or have your hours reduced. Private sector and state or local government employers with 20 or more employees offer COBRA continuation coverage. Wait for a letter in the mail. Elect health coverage within 60 days. Make a payment within 45 days.
You may be eligible to apply for individual coverage through Covered California, the State's Health Benefit Exchange. You can reach Covered California at (800) 300-1506 or online at www.coveredca.com. You can apply for individual coverage directly through some health plans off the exchange.
You may be eligible to apply for individual coverage through Covered California, the State's Health Benefit Exchange. You can reach Covered California at (800) 300-1506 or online at www.coveredca.com. You can apply for individual coverage directly through some health plans off the exchange.
You must meet three basic requirements to be entitled to elect COBRA continuation coverage: Your group health plan must be covered by COBRA; 2022 A qualifying event must occur; and 2022 You must be a qualified beneficiary for that event.
COBRA continuation coverage lets you stay on your employer's group health insurance plan after leaving your job. COBRA stands for the Consolidated Omnibus Budget Reconciliation Act. It's shorthand for the law change that required employers to extend temporary group health insurance to departing employees.
Actual notice. Constructive notice. Funding Opportunity Announcement. Judicial notice. Notice of Proposed Rulemaking (administrative law) Previous notice (parliamentary procedure) Public notice. Resign.
The word notice has to do with paying attention to something. For example, you usually notice a flashing light, and an overdue bill might come with the word "NOTICE" written on it to make sure you see it. The Latin n014dtitia, a noun meaning "something known," was the ancestor of notice.
SYNONYMS. observe, perceive, note, see, become aware of, discern, detect, spot, distinguish, catch sight of, make out, take notice of, mark, remark. pay attention to, take note of, heed, take heed of, pay heed to. British informal clock. literary behold, descry, espy.