Introductory COBRA Letter
What this document covers
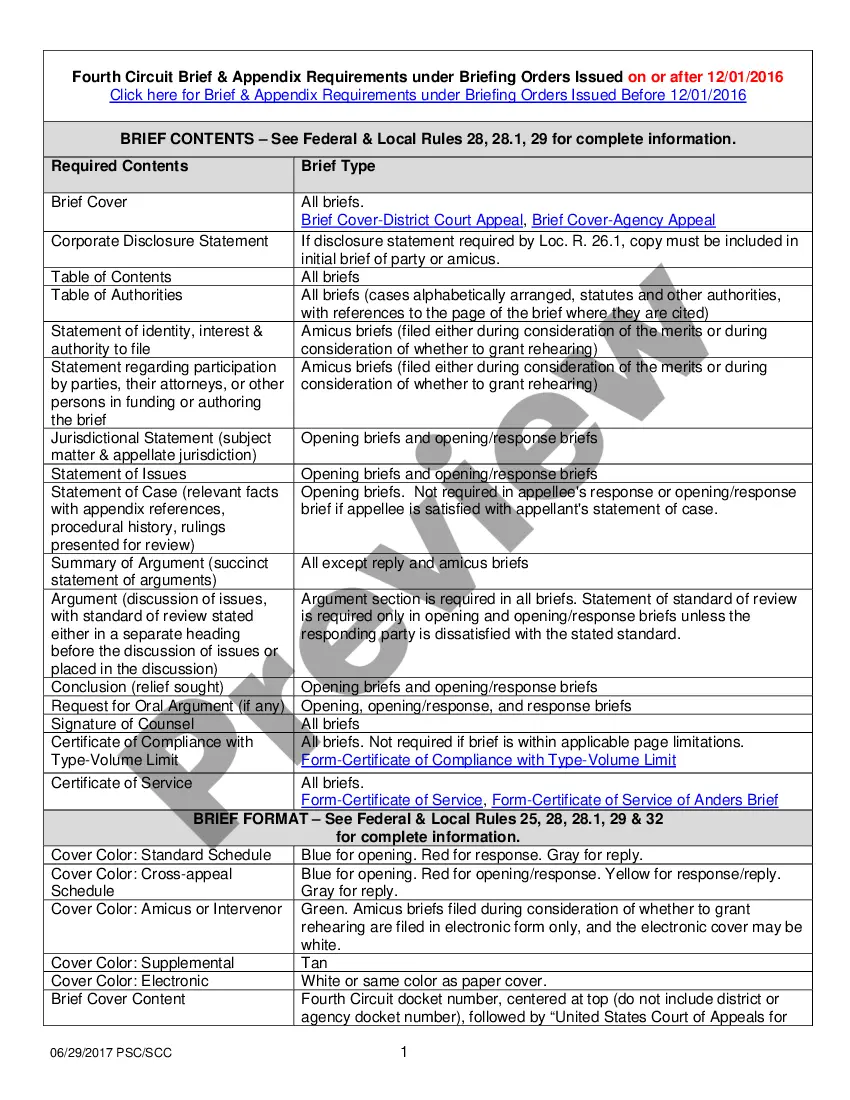
The Introductory COBRA Letter informs qualified beneficiaries about their rights to continued health care coverage under the Consolidated Omnibus Budget Reconciliation Act (COBRA). This form enables employers to formally notify eligible employees and their dependents about their coverage options, distinguishing it from other employment-related notification forms.
What’s included in this form
- Date of the letter
- Name and address of the qualified beneficiary
- Eligibility statement for health care coverage
- Details on coverage period and costs for individual and family plans
- Information on dependent coverage and conditions for discontinuation
- Instructions for completing and submitting the application
When this form is needed
This form should be used when an employee or their dependent qualifies for continued health care coverage under COBRA, typically after a qualifying event such as job loss, reduction in hours, or other circumstances that affect their health insurance eligibility. Employers must provide this letter promptly to ensure beneficiaries are aware of their rights and options.
Who this form is for
- Employers of any size who offer health care plans
- Human resources departments responsible for employee communications
- Eligible employees experiencing a qualifying event under COBRA
- Dependents of eligible employees who need information about their coverage
How to prepare this document
- Enter the date of the letter at the top.
- Fill in the name and address of the qualified beneficiary.
- Specify the monthly cost for individual and family coverage.
- Provide information regarding the application process and deadlines.
- Sign the letter in the section designated for the Human Resources Manager.
Does this document require notarization?
This form usually doesn’t need to be notarized. However, local laws or specific transactions may require it. Our online notarization service, powered by Notarize, lets you complete it remotely through a secure video session, available 24/7.
Get your form ready online
Our built-in tools help you complete, sign, share, and store your documents in one place.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.
Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.
Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.

Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.

Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Avoid these common issues
- Failing to include the correct names and addresses of beneficiaries.
- Omitting or incorrectly entering the coverage cost details.
- Not providing clear instructions for submitting the application.
- Neglecting to send the letter promptly after a qualifying event.
Benefits of using this form online
- Immediate access to professionally drafted letter templates.
- Easy customization to fit specific circumstances and ensure compliance.
- Ability to download and print directly for distribution.
- Secure and reliable storage of legal documents in digital format.
Quick recap
- The Introductory COBRA Letter is essential for notifying eligible employees of their health coverage rights.
- It includes critical details like coverage costs and application deadlines.
- Using this form helps ensure compliance with federal regulations while offering clarity to beneficiaries.
Looking for another form?
Form popularity
FAQ
Assuming one pays all required premiums, COBRA coverage starts on the date of the qualifying event, and the length of the period of COBRA coverage will depend on the type of qualifying event which caused the qualified beneficiary to lose group health plan coverage.
COBRA provides the same benefits as your employer-sponsored plan. COBRA limits you to 18 months of coverage though. You can request an 18-month extension if you or a dependent is disabled. You can also request one if you face another qualifying event, such as a spouse's death.
Contact The Employer's COBRA Plan AdministratorIf your employer can not answer your questions or does not comply, you can call the Department of Labor at 1-866-487-2365.
COBRA continuation coverage notices are documents that explain employees' rights under the Consolidated Omnibus Budget Reconciliation Act of 1985.Details on who qualifies for COBRA coverage and what they must do to obtain coverage. A reminder to tell the plan administrator of any address or beneficiary changes.
Q8: How long do I have to elect COBRA coverage? If you are entitled to elect COBRA coverage, you must be given an election period of at least 60 days (starting on the later of the date you are furnished the election notice or the date you would lose coverage) to choose whether or not to elect continuation coverage.
You may be eligible to apply for individual coverage through Covered California, the State's Health Benefit Exchange. You can reach Covered California at (800) 300-1506 or online at www.coveredca.com. You can apply for individual coverage directly through some health plans off the exchange.
Separate requirements apply to the employer and the group health plan administrator. An employer that is subject to COBRA requirements is required to notify its group health plan administrator within 30 days after an employee's employment is terminated, or employment hours are reduced.
Notices properly mailed are generally considered provided on the date sent, regardless of whether they're actually received. 1. COBRA Initial Notice must be provided. Within 30 days after the employee first becomes enrolled in the group health plan.
You'll have 60 days to enroll in COBRA or another health plan once your benefits end. But keep in mind that delaying enrollment won't save you money. COBRA is always retroactive to the day after your previous coverage ends, and you'll need to pay your premiums for that period too.