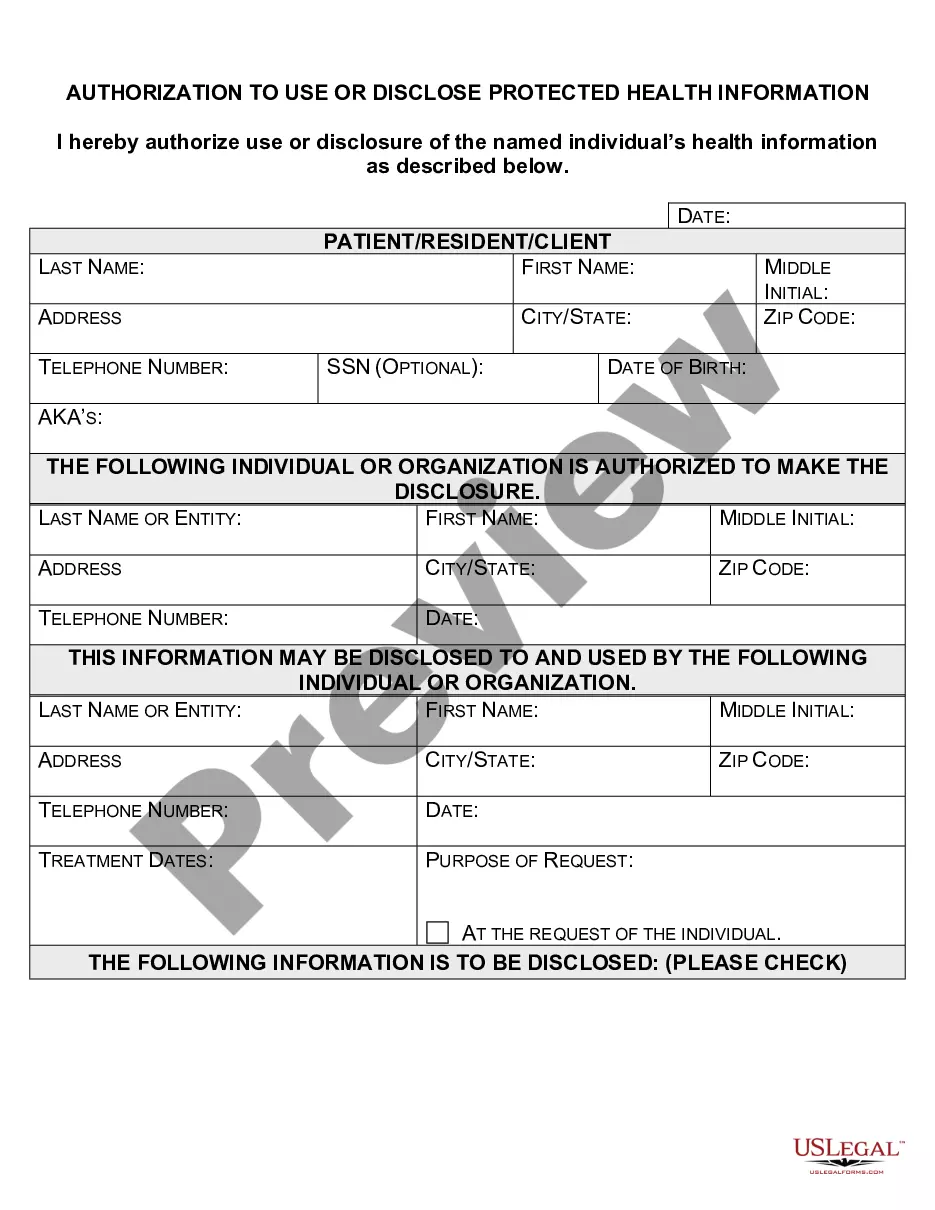
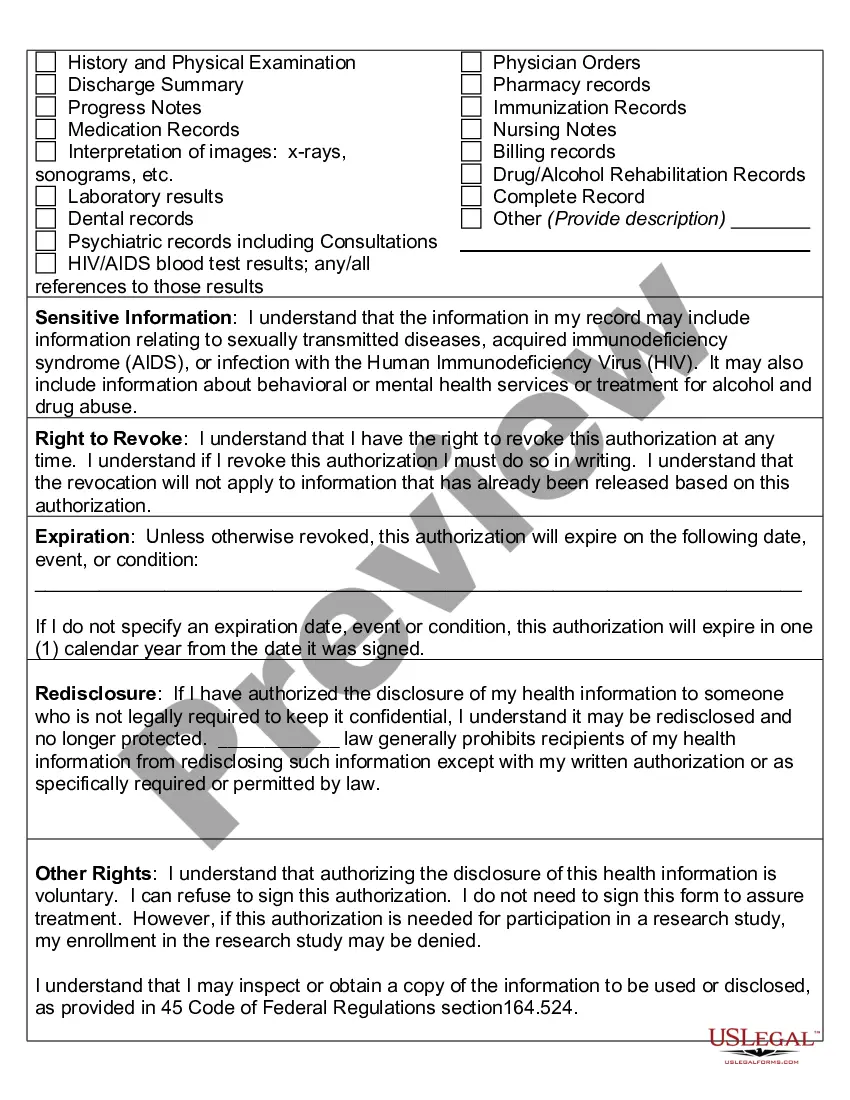
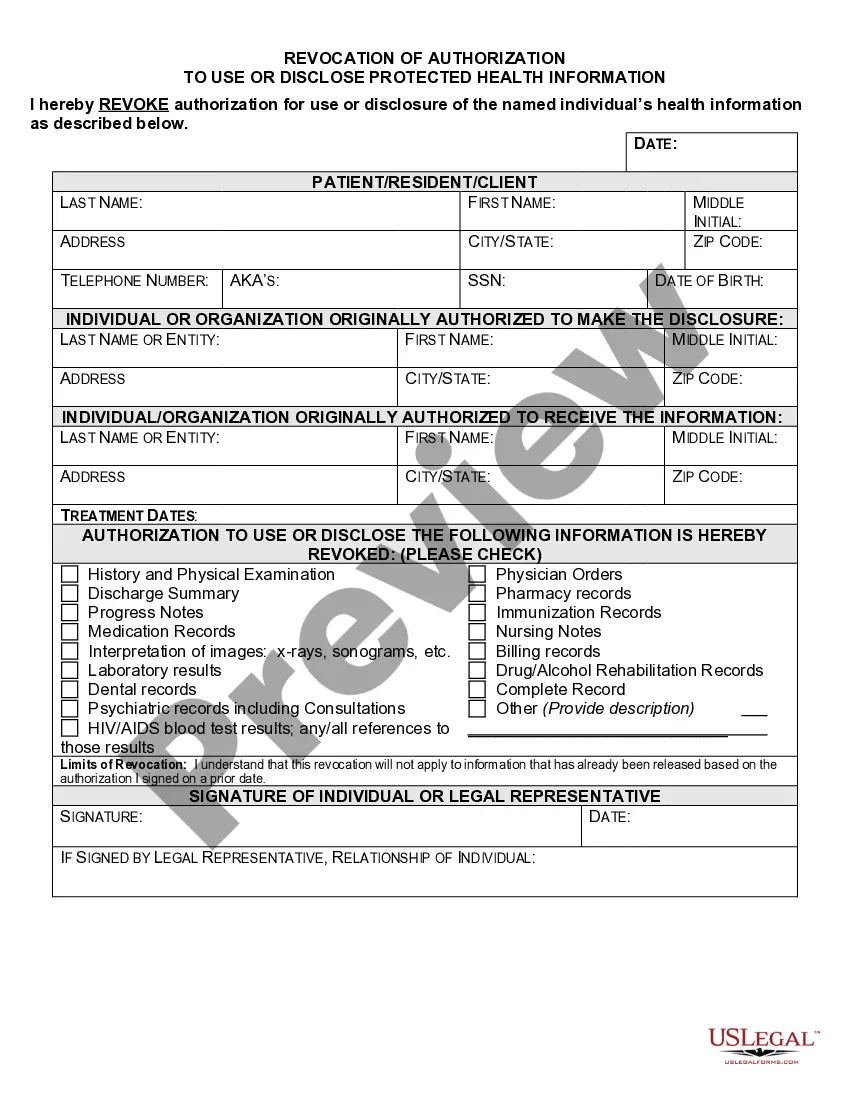
Montana Authorization to Use or Disclose Protected Health Information
Description
How to fill out Authorization To Use Or Disclose Protected Health Information?
It is feasible to spend hours online attempting to locate the valid document template that complies with the federal and state criteria you will require.
US Legal Forms offers a vast array of valid forms that can be reviewed by professionals.
You can conveniently download or print the Montana Authorization to Use or Disclose Protected Health Information from my service.
If available, utilize the Preview button to look through the document format as well.
- If you already possess a US Legal Forms account, you can Log In and press the Obtain button.
- Then, you can complete, edit, print, or sign the Montana Authorization to Use or Disclose Protected Health Information.
- Every valid document template you acquire is yours indefinitely.
- To obtain another copy of the purchased form, visit the My documents section and click the appropriate button.
- If you are using the US Legal Forms website for the first time, follow the simple instructions below.
- First, ensure you have selected the correct document format for your region/area that you choose.
- Check the form description to verify you have selected the right form.
Form popularity
FAQ
In limited circumstances, the HIPAA Privacy Rule permits covered entities to use and disclose health information without individual authorization. Covered entities may use and disclose protected health information without authorization for their own treatment, payment, and healthcare operations.
Covered entities may disclose protected health information that they believe is necessary to prevent or lessen a serious and imminent threat to a person or the public, when such disclosure is made to someone they believe can prevent or lessen the threat (including the target of the threat).
What are two required elements of an authorization needed to disclose PHI? Response Feedback: All authorizations to disclose PHI must have an expiration date and provide an avenue for the patient to revoke his or her authorization. What does the term "Disclosure" mean?
Valid HIPAA Authorizations: A ChecklistNo Compound Authorizations. The authorization may not be combined with any other document such as a consent for treatment.Core Elements.Required Statements.Marketing or Sale of PHI.Completed in Full.Written in Plain Language.Give the Patient a Copy.Retain the Authorization.
An authorization must specify a number of elements, including a description of the protected health information to be used and disclosed, the person authorized to make the use or disclosure, the person to whom the covered entity may make the disclosure, an expiration date, and, in some cases, the purpose for which the
A HIPAA authorization is a detailed document in which specific uses and disclosures of protected health are explained in full. By signing the authorization, an individual is giving consent to have their health information used or disclosed for the reasons stated on the authorization.
The HIPAA Privacy Rule requires that an individual provide signed authorization to a covered entity, before the entity may use or disclose certain protected health information (PHI).
A patient authorization is not required for disclosure of PHI between Covered Entities if the disclosure is needed for purposes of treatment or payment or for healthcare operations. You may disclose the PHI as long as you receive a request in writing.
In general, a covered entity may only use or disclose PHI if either: (1) the HIPAA Privacy Rule specifically permits or requires it; or (2) the individual who is the subject of the information gives authorization in writing.
However, PHI can be used and disclosed without a signed or verbal authorization from the patient when it is a necessary part of treatment, payment, or healthcare operations. The Minimum Necessary Standard Rule states that only the information needed to get the job done should be provided.