The parties may agree to a different performance. This is called an accord. When the accord is performed, this is called an accord and satisfaction. The original obligation is discharged. In order for there to be an accord and satisfaction, there must be a bona fide dispute; an agreement to settle the dispute; and the performance of the agreement. An example would be settlement of a lawsuit for breach of contract. The parties might settle for less than the amount called for under the contract.
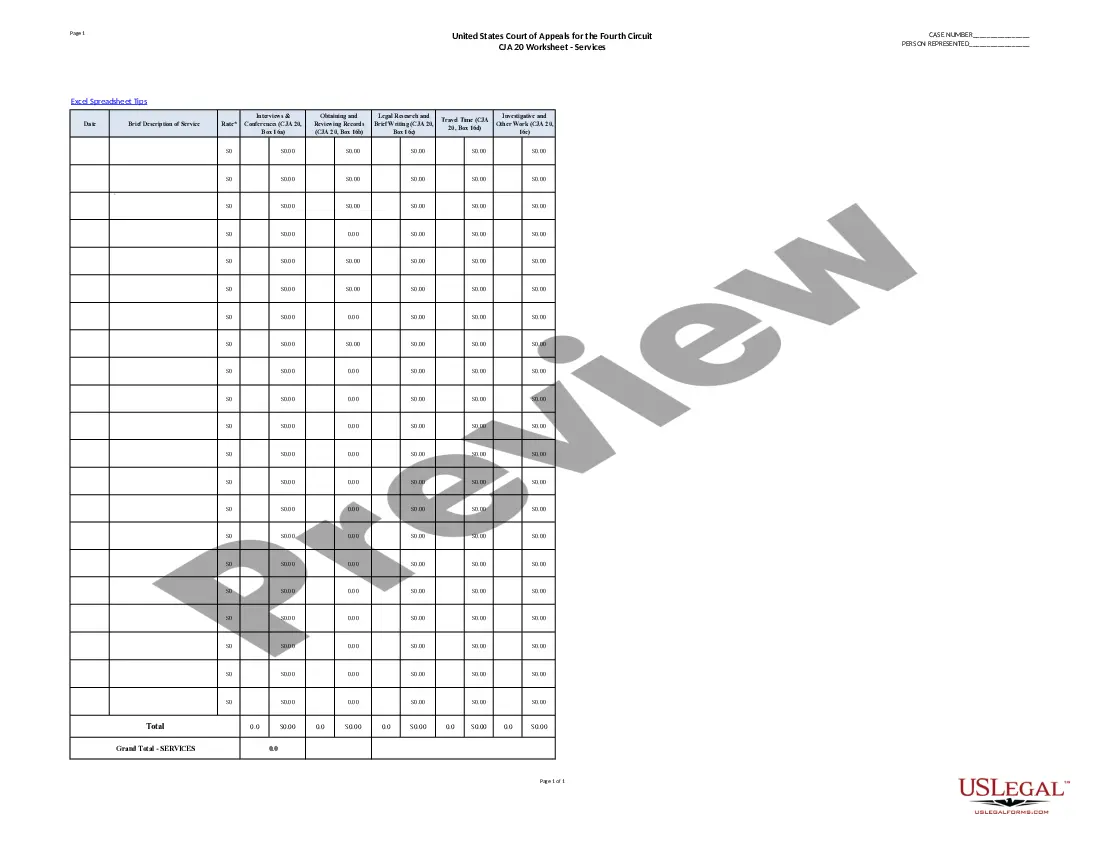
Here Denied Claim For Capitation In Texas
Description
Get your form ready online
Our built-in tools help you complete, sign, share, and store your documents in one place.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.
Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.
Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.

Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.

Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Looking for another form?
Form popularity
FAQ
Denial code 197 means that the precertification, authorization, notification, or pre-treatment requirement was not fulfilled or was absent.
Denial code 22 is when the healthcare service may be covered by another insurance provider due to coordination of benefits.
What is Denial Code 23. Denial code 23 is used to indicate that the claim has been denied due to the impact of prior payer(s) adjudication, which includes payments and/or adjustments. This denial code is typically used in conjunction with Group Code OA.
NPS Reason Code 22 is one of the common issues users face when using the Extensible Authentication Protocol (EAP) type on the client's computer. In short, it typically means that NPS could not complete the EAP handshake with the client device, usually because NPS or the client were misconfigured.
This denial means that the claim was denied because the charges are covered under a capitation agreement or managed care plan - in this case, the Medicare Advantage plan.
Adjusted Service lines Report Shows claims that have a status of 22 (reversal of previous payment). This report does not show the adjustment claim that reflects the corrected dollar amounts, but shows only the negative amount that the reversed claim provides to negate the original claim.
Causes of a Code 22 Error In most cases, it means the device was manually disabled, but you might also see it if Windows is forced to disable the device due to a lack of system resources. Details on error codes like this one are available from the device status area of a device's properties in Device Manager.
Most Texas Medicaid and CHIP members receive their services through a managed care organization (MCO). The four main Medicaid programs are: STAR, STAR Health, STAR Kids and STAR+PLUS.
Benefits include: Primary care provider visits. Prescription drugs. Immunizations and wellness visits. Specialist visits. Urgent care. Emergency care. Lab and X-ray services. Pregnancy services.
The CO 24 denial code is used to indicate that the claim made has been denied due to the patient's insurance coverage under a capitation agreement or a managed care plan.