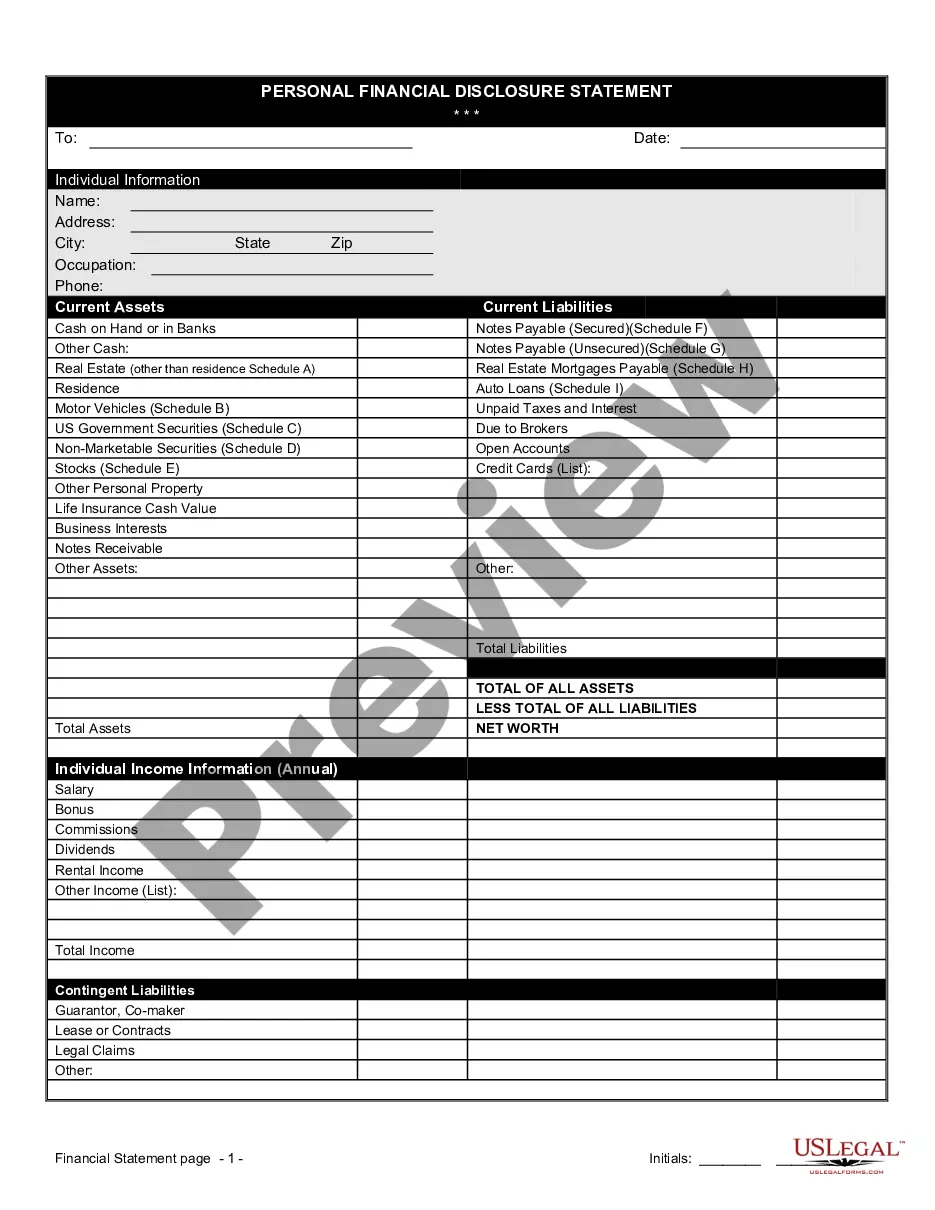
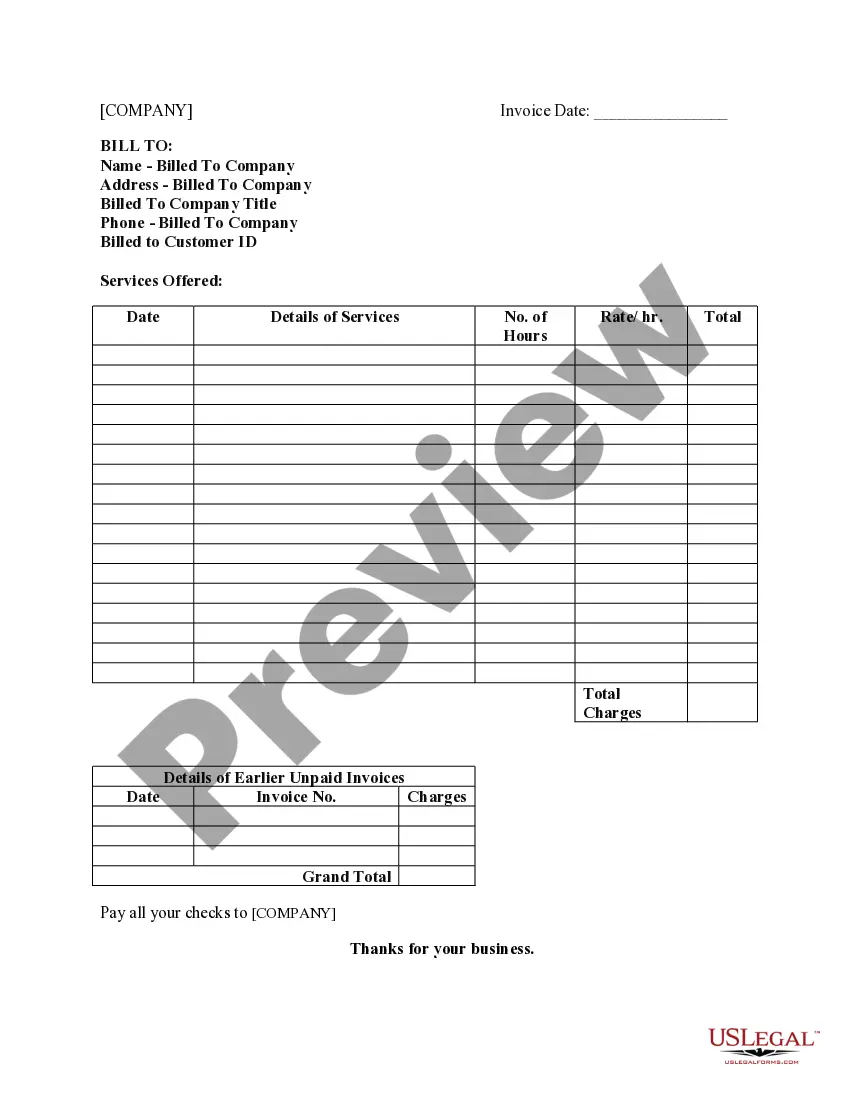
Notice of Special Enrollment Rules
Understanding this form
The Notice of Special Enrollment Rules is a legal document that informs individuals about their rights to enroll in health insurance coverage under specific circumstances. This form is essential for those who may have declined enrollment due to existing health insurance. Unlike standard enrollment forms, this notice clarifies the special rules that allow enrollment outside the usual open enrollment period.
Key components of this form
- Indication of whether enrollment is declined due to other health coverage.
- Details about the 30-day period for requesting enrollment after other coverage ends.
- Information regarding eligibility for new dependents due to marriage, birth, adoption, or placement for adoption.
When to use this document
This form should be used when an individual declines health insurance enrollment due to being covered by another plan. It is also necessary when a new dependent is added due to significant life events, such as marriage or the birth of a child. In both situations, this notice must be submitted within 30 days after the qualifying event.
Intended users of this form
This form is intended for:
- Individuals who have declined health insurance enrollment due to existing coverage.
- Parents who need to enroll their children after a birth or adoption.
- Spouses newly added as dependents after marriage.
Completing this form step by step
- Identify the individuals who are enrolling, including yourself and any dependents.
- Specify the reason for initiating enrollment based on the qualifying event.
- Enter the dates regarding the end of previous coverage or the occurrence of a new dependent event.
- Provide any necessary documentation that supports your request.
- Submit the completed form within 30 days of the event to ensure enrollment eligibility.
Notarization requirements for this form
This form usually doesn’t need to be notarized. However, local laws or specific transactions may require it. Our online notarization service, powered by Notarize, lets you complete it remotely through a secure video session, available 24/7.
Get your form ready online
Our built-in tools help you complete, sign, share, and store your documents in one place.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.
Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.
Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.

Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.

Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Avoid these common issues
- Failing to submit the form within the 30-day deadline.
- Not providing adequate documentation for qualifying events.
- Forgetting to include all dependents who need to be enrolled.
Advantages of online completion
- Convenience of downloading and completing the form at your convenience.
- Editability allows for quick changes if your situation changes.
- Access to clear instructions enhances the likelihood of successful submission.
Legal use & context
- This notice serves as an official record of your eligibility for special enrollment.
- It is essential to safeguard your rights under health insurance regulations.
- Utilizing this form helps in complying with health insurance marketplace requirements.
Key takeaways
- The Notice of Special Enrollment Rules is vital for understanding your health insurance options after specific events.
- Enrollment must be requested within 30 days following the loss of prior coverage or when a new dependent arrives.
- Filling out the form correctly is essential to secure necessary health insurance coverage.
Looking for another form?
Form popularity
FAQ
You may qualify for a Special Enrollment Period to enroll any time if you've had certain life events, including losing health coverage, moving, getting married, having a baby, or adopting a child.
Under HIPAA, special enrollment rights allow eligible employees and/or dependents to enroll in an employer-sponsored group medical plan during the plan year, due to certain events.Loss of eligibility under other medical plan coverage due to: termination of employment or reduction in hours.
The second type of qualifying events are the optional events under Section 125: Change in status (employment, marital status, number of dependents, residence) Change in cost (significant and insignificant) Significant coverage curtailment
Special enrollment allows individuals who previously declined health coverage to enroll for coverage.Under the first, employees and dependents who decline coverage due to other health coverage and then lose eligibility or lose employer contributions have special enrollment rights.
If you miss your employer's open enrollment deadline, you could lose coverage for you and your loved ones, and you could be subject to a fine imposed by the Affordable Care Act (ACA). Missing this deadline also means that you could be unable to make changes or enroll in benefits until the next open enrollment period.
If you miss your employer's open enrollment deadline, you could lose coverage for you and your loved ones, and you could be subject to a fine imposed by the Affordable Care Act (ACA). Missing this deadline also means that you could be unable to make changes or enroll in benefits until the next open enrollment period.
The Affordable Care Act (ACA) no longer requires everyone to have health coverage. You will not have to pay a tax penalty if you missed open enrollment and don't have coverage for 2020. However, going without health insurance could leave you at risk for high unexpected medical bills.
You may qualify for a Special Enrollment Period if you or anyone in your household lost qualifying health coverage in the past 60 days (or more than 60 days ago but since January 1, 2020) OR expects to lose coverage in the next 60 days.
You usually have 30 to 60 days to enroll in a health plan after a qualifying event. If you expect to lose health insurance coverage within the next 60 days, like if you know you will leave your job, you may even have access to a Special Enrollment Period before your qualifying event.