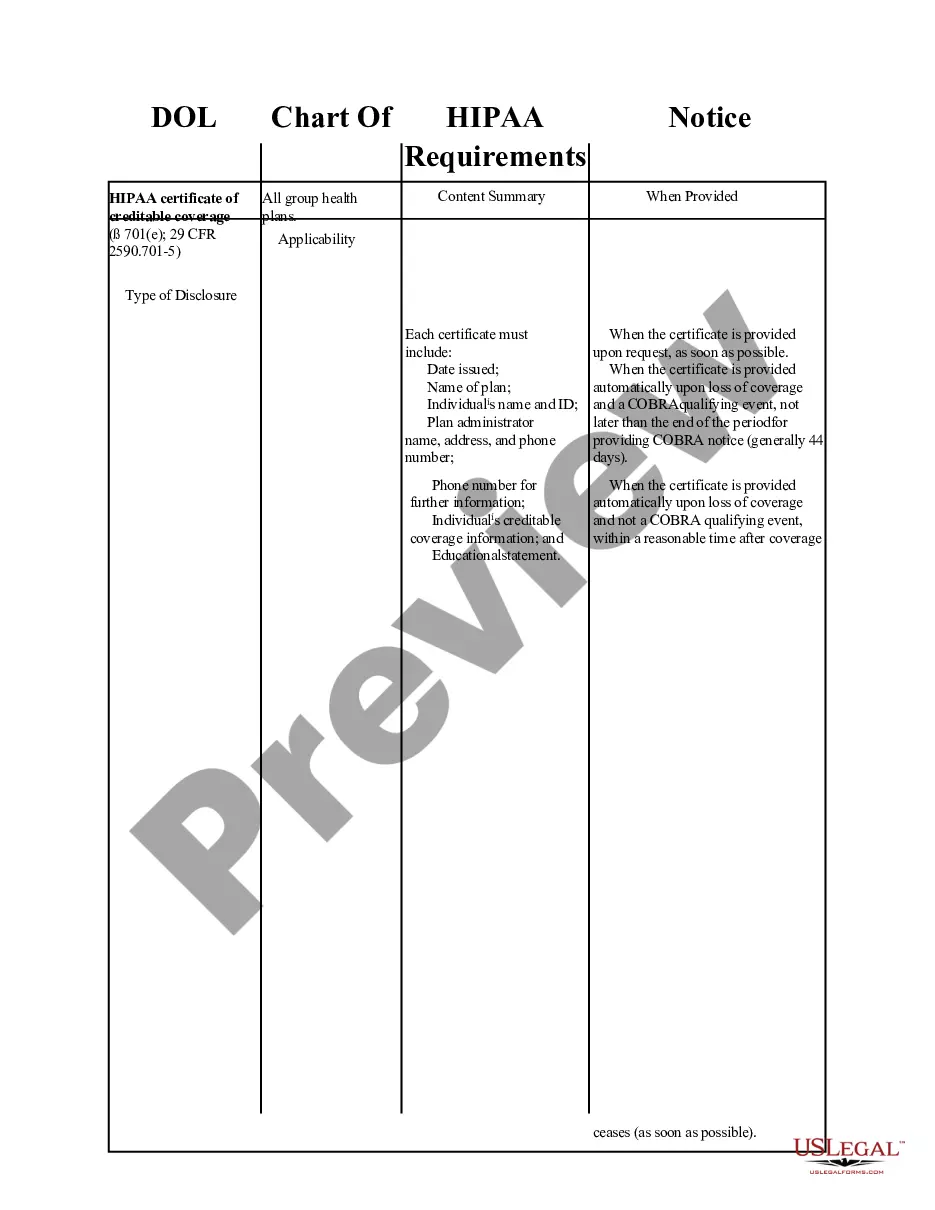
HIPAA Certification Requirements
What is this form?
The HIPAA Certification Requirements form is a crucial document designed to outline the specific certification requirements that group health plans must adhere to under the Health Insurance Portability and Accountability Act (HIPAA). This form differentiates itself from other health-related forms by focusing specifically on the rules related to preexisting conditions, enrollment periods, and requirements for creditable coverage, ensuring that health coverage is portable and accessible.
What’s included in this form
- Definition of preexisting condition exclusions and their limitations.
- Guidelines for creditable coverage regarding various health plans.
- Details on special enrollment periods available under HIPAA.
- Certification requirements for prior creditable coverage documentation.
- Information on the rights of individuals regarding health insurance and discrimination.
When to use this form
This form should be used when a group health plan administrator needs to ensure compliance with HIPAA guidelines during the enrollment process. It is most relevant when an employee is onboarding to a new employer, qualifying for special enrollment, or when an individual is transitioning between health plans. It is also required when assessing if preexisting condition exclusions apply to individuals based on their previous health coverage.
Who this form is for
- Group health plan administrators managing employee health benefits.
- Employees enrolling in group health plans who need to verify and document prior health coverage.
- Individuals transitioning between health plans and requiring proof of creditable coverage.
Steps to complete this form
- Identify the specific provisions of HIPAA that apply to your group health plan.
- Gather relevant documentation demonstrating creditable coverage from previous health plans.
- Complete the required certification details, including the participant's information and plan specifics.
- Ensure that all certification statements reflect accurate information regarding preexisting conditions and enrollment.
- Provide written certification to participants when they cease coverage or become eligible for COBRA.
Notarization guidance
This form does not typically require notarization unless specified by local law. However, obtaining notarization may provide additional assurance regarding the legitimacy of the certifications. Always verify any specific requirements based on your state's regulations.
Get your form ready online
Our built-in tools help you complete, sign, share, and store your documents in one place.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.
Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.
Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.

Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.

Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Common mistakes to avoid
- Failing to document prior coverage accurately, which can lead to unnecessary exclusions.
- Not providing required certifications in a timely manner.
- Overlooking the specifics of preexisting conditions and their limitations.
Why use this form online
- Convenient access to compliant HIPAA certification forms anytime.
- Editability allows plan administrators to customize the form as needed.
- Reliable, attorney-drafted templates ensure adherence to legal requirements.
Legal use & context
- This form serves to enforce the individual rights established under HIPAA regarding health coverage portability.
- It is essential for group health plans to comply with federal regulations and to avoid penalties.
- Understanding the nuances of creditable coverage can prevent potential disputes with insurers.
Key takeaways
- The HIPAA Certification Requirements form is crucial for group health plans to outline coverage standards.
- Accurate completion is essential for ensuring compliance and protecting individual rights related to health coverage.
- Utilizing the form properly can aid in navigating the complexities of health insurance transitions.
Looking for another form?
Form popularity
FAQ
Nonetheless, despite there being no requirement for HIPAA certification, some companies claim to be certified as HIPAA compliant.
A breach is defined in HIPAA section 164.402, as highlighted in the HIPAA Survival Guide, as: The acquisition, access, use, or disclosure of protected health information in a manner not permitted which compromises the security or privacy of the protected health information.
Implement Access Control requirements. Implement Person or Entity Authentication requirements. Implement the Transmission Security requirements. Disposal as a Requirement. The Data Backup and Storage Implementation. Integrity as a Feature.
HIPAA compliance training will educate employees about what HIPAA is, why it is so important and how to honor its guidelines. This means learning about what PHI is, how to recognize it and when it can be transmitted without patient authorization.
According to the Privacy Rule, HIPAA training is required for each new member of the workforce within a reasonable period of time after the person joins the Covered Entity's workforce and also when functions are affected by a material change in policies or procedures again within a reasonable period of time.
With a lot of changes happening to the health care industry and HIPAA rules, currently, the certificate is valid for 1 year. You will NOT be required to take any new test after the year only a paid update course (if rule changes) will be needed.
HIPAA requires that both covered entities and business associates provide HIPAA training to members of their workforce who handle PHI.Business associates and any of their subcontractors must have training. Basically, anyone who comes into contact with protected health information (PHI) must be trained.
Although there is no official HHS-mandated HIPAA certification process or accreditation, it would be beneficial if there was.Nonetheless, despite there being no requirement for HIPAA certification, some companies claim to be certified as HIPAA compliant.
The three components of HIPAA security rule compliance. Keeping patient data safe requires healthcare organizations to exercise best practices in three areas: administrative, physical security, and technical security.