COBRA Notice Timing Delivery Chart
What is this form?
The COBRA Notice Timing Delivery Chart is a crucial document for employers and plan administrators to ensure compliance with the Consolidated Omnibus Budget Reconciliation Act of 1985 (COBRA). This form outlines the timing and delivery requirements for various COBRA notices, helping to clarify obligations during qualifying events that can affect health insurance coverage. Unlike other forms, this chart serves as a reference tool rather than a notice itself, providing a structured overview of key timelines and methods of notification.
Key components of this form
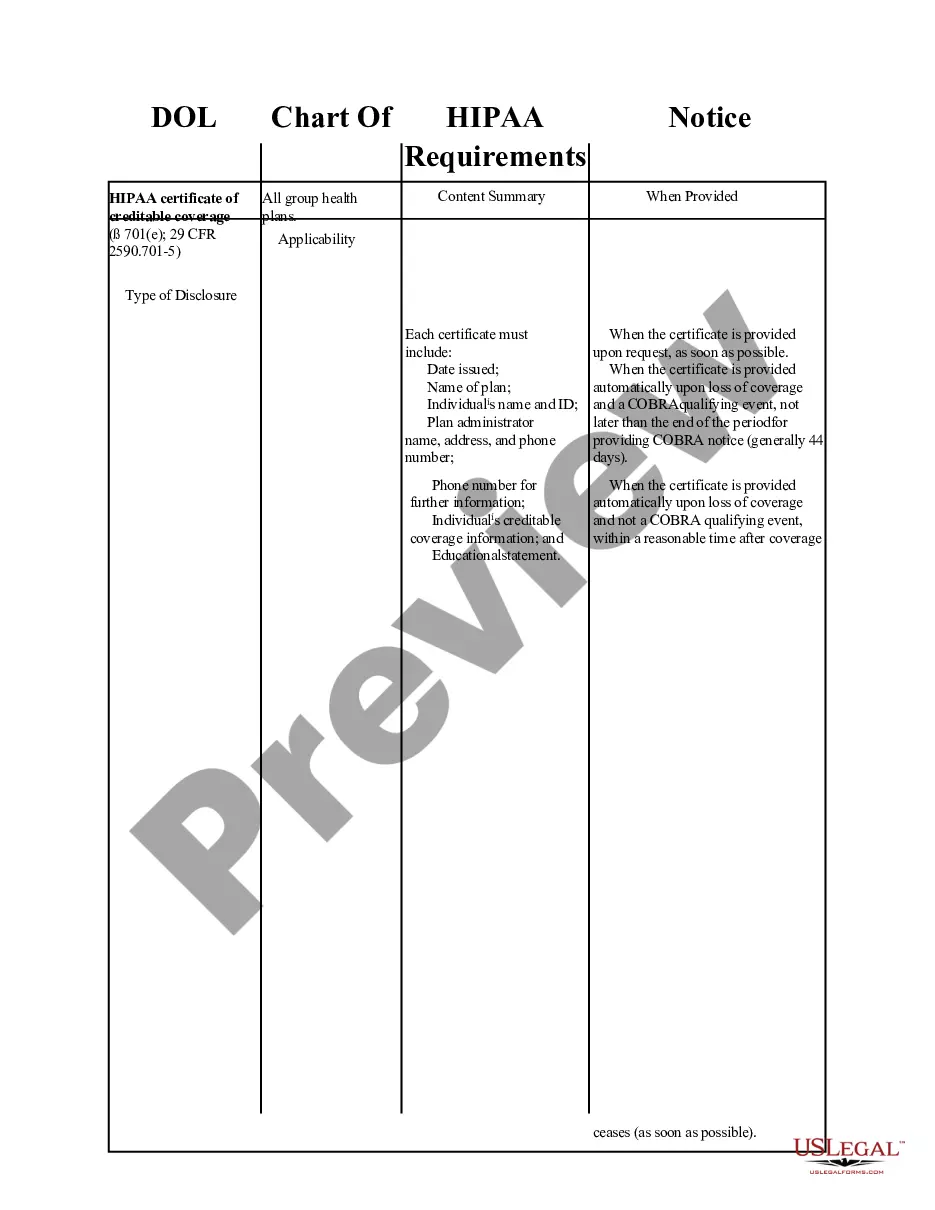
- Notice Description: Details regarding the type of notice and its purpose.
- Timing: Specifies the deadlines for issuing various COBRA notices.
- Delivery Methods: Outlines acceptable methods for delivering notices (e.g., mail, electronic notification).
- Responsibilities: Clarifies who is responsible for sending notices (e.g., employers, plan administrators).
- Qualified Beneficiaries: Identifies who qualifies for notifications under COBRA.
When this form is needed
This form should be utilized by employers and plan administrators when managing COBRA compliance, particularly during qualifying events such as employee termination, reduction of hours, or other significant changes in health coverage eligibility. It serves as a reference for ensuring that all necessary notices are delivered timely and to the correct individuals.
Who this form is for
- Employers who sponsor group health plans.
- Plan administrators responsible for issuing COBRA notices.
- Human resources professionals overseeing employee benefits.
- Legal or compliance officers ensuring COBRA regulations are met.
How to prepare this document
- Review the specific types of COBRA notices and their purposes as outlined in the chart.
- Identify the timing requirements for each notice based on qualifying events.
- Select appropriate delivery methods for sending notices to qualified beneficiaries.
- Assign responsibilities to ensure notices are delivered on time.
- Keep documentation of all notices sent for compliance verification.
Does this form need to be notarized?
This form does not typically require notarization to be legally valid. However, some jurisdictions or document types may still require it. US Legal Forms provides secure online notarization powered by Notarize, available 24/7 for added convenience.
Get your form ready online
Our built-in tools help you complete, sign, share, and store your documents in one place.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.
Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.
Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Make edits, fill in missing information, and update formatting in US Legal Forms—just like you would in MS Word.

Download a copy, print it, send it by email, or mail it via USPS—whatever works best for your next step.

Sign and collect signatures with our SignNow integration. Send to multiple recipients, set reminders, and more. Go Premium to unlock E-Sign.
If this form requires notarization, complete it online through a secure video call—no need to meet a notary in person or wait for an appointment.
We protect your documents and personal data by following strict security and privacy standards.
Common mistakes to avoid
- Failing to send notices within the specified timeframes.
- Not delivering notices to all qualified beneficiaries.
- Using incorrect methods of delivery as dictated by COBRA regulations.
- Overlooking changes in a beneficiary's status that require updated notices.
- Assuming verbal notifications are sufficient without written documentation.
Advantages of online completion
- Convenience: Access the form instantly from anywhere with internet access.
- Editability: Easily modify the form to include specific details related to your organization.
- Reliability: Utilize a standardized chart crafted by legal professionals, ensuring compliance with COBRA regulations.
- Record keeping: Maintain a digital copy for your records and future reference.
Legal use & context
- The COBRA Notice Timing Delivery Chart is essential for legal compliance in administering COBRA rights.
- Failure to provide timely notices can lead to penalties and legal challenges for employers.
- Using this form helps ensure that all parties are properly informed about their rights regarding health coverage after qualifying events.
What to keep in mind
- The COBRA Notice Timing Delivery Chart is essential for compliance with federal laws.
- Understanding the key components can help prevent costly mistakes.
- Employers and plan administrators are responsible for timely and accurate notifications to qualified beneficiaries.
Looking for another form?
Form popularity
FAQ
Your employer must mail you the COBRA information and forms within 14 days after receiving notification of the qualifying event. You are responsible for making sure your COBRA coverage goes into and stays in effect - if you do not ask for COBRA coverage before the deadline, you may lose your right to COBRA coverage.
An employer that is subject to COBRA requirements is required to notify its group health plan administrator within 30 days after an employee's employment is terminated, or employment hours are reduced.
Notices properly mailed are generally considered provided on the date sent, regardless of whether they're actually received. 1. COBRA Initial Notice must be provided. Within 30 days after the employee first becomes enrolled in the group health plan.
Employers should send notices by first-class mail, obtain a certificate of mailing from the post office, and keep a log of letters sent. Certified mailing should be avoided, as a returned receipt with no delivery acceptance signature proves the participant did not receive the required notice.
COBRA Coverage Timeline An employee who's eligible for Consolidated Omnibus Budget Reconciliation Act (COBRA) coverage must elect it within 60 days of their insurance termination date, or the date that the employee recieved their COBRA notification, whichever is later.
The insurance company. COBRA Election Notice. After receiving a notice of a qualifying event, the plan must provide the qualified beneficiaries with an election notice within 14 days. The election notice describes their rights to continuation coverage and how to make an election.
The employer must notify the plan within 30 days of the event. You (the covered employee or one of the qualified beneficiaries) must notify the plan if the qualifying event is divorce, legal separation, or a child's loss of dependent status under the plan.